Osteonecrosis of the jaw
What is osteonecrosis of the jaw? Osteonecrosis (ONJ) is a rigorous disease of the bone that affects the upper and lower jaws.
Although the condition is uncommon, bisphosphonate-associated osteonecrosis of the jaw is a known concern in people being treated for osteoporosis; especially those who have had recent dental work.
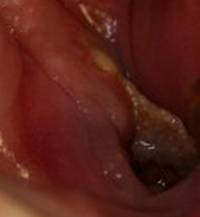
Osteonecrosis of the Jaw Symptoms
The main signs and symptoms of jaw necrosis include exposed bone – that does not heal, pain, gum infection, poor healing of gums, loose teeth, and numbness in the jaw.
Osteonecrosis Risk Groups
There are two major risk groups of jaw necrosis that relate to bisphosphonate use.
- High dose Intravenous bisphosphonate use in cancer patients
- Bisphosphonate use in people who have had recent dental work
There is a strong relationship between the use of high dose bisphosphonates treatments – such as used in the treatment of plasma cell myeloma and breast cancer – and jaw osteonecrosis. In a study carried out in Germany, 97% of all cases of bisphosphonates relating to necrosis of the jaw occurred in cancer patients taking high dosages of intravenous bisphosphonates such as zoledronate and pamidronate. It has been reported by the IMF that the incidence of osteonecrosis in cancer sufferers undergoing this specialized treatment can be as high 10% (zoledronate acid).
There is a very strong link between dental surgery, especially tooth extraction, and the use of bisphosphonates. It is estimated that 73% of all osteoporosis bisphosphonates and jaw necrosis related cases occur in people who have had dental treatments such as tooth extraction and root canal treatment.
It is therefore of the utmost importance that people are considered to be ‘dentally fit’, and given instruction on how to maintain healthy teeth through oral hygiene, before they are considered for a course of bisphosphonates for the treatment of osteoporosis.
Bisphosphonates and Jaw Necrosis in People with Osteoporosis
There is a large difference in the incidence of jaw osteonecrosis in people taking intravenous bisphosphonates and oral bisphosphonate. As mentioned previously the rates of osteonecrosis can reach as high as 10% in myeloma sufferers being treated with zoledronate acid. The incidence of osteonecrosis in the general population is much lower:
- Oral bisphosphonate osteonecrosis of the jaw incidence rate ≈0.04%
- Intravenous bisphosphonate osteonecrosis jaw rate ≈ 1.15%
To put this in perspective if you are being treated for osteoporosis only (not a cancer related treatment), a study in Germany revealed that the risk of osteonecrosis was ≈ 0.0004% or ≈ 4 per million people being treated for the condition.
Why Does Bisphosphonates Use Lead to Jaw Osteonecrosis
One of the reasons that bisphosphonates can cause jaw necrosis is a consequence of the make up of the maxilla (upper jaw) and mandible (lower jaw) bones. The unique environment of the jaw can lead to cavities forming through prolonged bisphosphonate use. These can compromise the blood supply to the bones. Upon dental treatment, the open wound cannot heal correctly, leaving it susceptible to infections by oral microbiota. These infections lead to an inflammation of the bone (osteomyelitis), which in turn leads to osteonecrosis. The reason that bone necrosis does not commonly occur in other parts of the skeleton is because they are enclosed areas, and therefore unlikely to come into contact with microbiota.
Osteonecrosis of the Jaw Treatment
So what happens if you are taking bisphosphonates and have a non-healing wound? The first thing will be a thorough examination by your dentist to confirm whether you have ‘bis-phossy’ jaw (other conditions such as diabetes and radiology can also lead to non-healing wounds).
Once bisphosphonate related osteonecrosis of the jaw has been confirmed the dentist is likely to have a consultation with your doctor, and it is possible that that you will be told to stop taking bisphosphonates.
The dentist is very unlikely to take out any major surgical work until at least three months, sometimes longer, after bisphosphonate use has ceased.
In the meantime, your condition is likely to be monitored, and antiseptic mouth washes and antibiotics used to prevent bacterial infections of the wound. This may well be the only form of osteonecrosis of the jaw treatment that is required – given time the bone may become covered with new mucosal; this is likely to be a slow progress.
If the condition is very painful and/or there is a lot of secondary infection, then the use of localized surgical debridement and bone grafting may be considered necessary.
Summary
The use of bisphosphonates in the treatment of osteoporosis is well tolerated by most people. However, the risk of osteonecrosis of the jaw is a concern that many people have when considering to use the drug or not. It is recommended that a person is given a thorough dental examination and declared to be ‘dentally fit’ and instructed on correct dental hygiene procedures before partaking on a course of bisphosphonates therapy.