What is Osteoporosis?
Osteoporosis Information: An Overview of the Bone Strength Affecting Skeletal Disorder
Osteoporosis is a condition in which bones become weaker and are more susceptible to fractures. The word itself comes from the two Greek words, ostoun and poros; these translate to bone and pore in English.
The condition is officially defined as ‘a skeletal disorder characterized by compromised bone strength predisposing a person to an increased risk of fracture’ (NIH Consensus Development Panel on Osteoporosis).
Unfortunately, many people do not realize that they are suffering from thinning bones until they have a fracture. This has led to osteoporosis becoming known as the ‘silent disease’.
The condition has also been described as a ‘a pediatric disease with geriatric consequence’. This is because peak bone formation and mass occurs during the teens (women 16–20), and the early twenties (men 20–25), yet any symptoms of a poor diet/lifestyle will not be seen until a person is much older.
Who Does Osteoporosis Affect – Some Facts and Figures
Osteoporosis can affect both men and women, though it is the latter who are at most risk. It is especially prevalent in postmenopausal women and the elderly. It is thought that globally from 33–50% (approximately 50% in the UK) of women over the age of fifty, and twenty percent of men, will be susceptible to an osteoporosis related fracture at some point in the remainder of their life.

Of the people hospitalized for an osteoporosis injury in the USA: 88.6% were women, and 11.4% were men. Close to 90% of these cases involved people aged over 65. The five most common injuries that led to hospitalization in people with osteoporosis were all fracture related (spontaneous and stress fractures being the most common at 29.5%).
Number of people with osteoporosis
As many people with osteoporosis remain undiagnosed until a fracture occurs it is difficult to know the exact number of people who suffer from the condition. It is estimated that from 20–40 million people suffer from osteoporosis in the United States, 3 million in the UK, and ~700,000 in Australia.
Costs of osteoporosis
- In the UK, over £2.3 billion is spent yearly on treating hip fractures.
- In the USA (2008), the estimated cost of total osteoporosis related treatment is $22 billion.
- In Australia (2004) AU$304 million was spent on the treatment of osteoporosis; of this AU$215 was spent on medication.
- In Canada (2010) the estimated yearly costs associated with the condition are CND$2.3 billion.
- Europe’s largest six economies (Germany, UK, France, Spain, Italy and Sweden) spent a combined €30.7 billion on the treatment of osteoporosis in 2010.
World Osteoporosis Statistics
As a person’s ethnic background is one of the known risk factors for osteoporosis it is little surprise that the prevalence of osteoporosis varies from region to region, as does the percentage of the location of the fracture site. The following table provides osteoporosis statistics that are based on data from the year 2000 provided by the WHO. At that time close to 9 million osteoporosis related fractures occurred in people aged 50 years or older.
| Region | Distribution of world osteoporotic fractures | Hip (percentage of fractures in region) | Spine (percentage of fractures in region) |
|---|---|---|---|
| Europe | 34.8% | 19.8% | 15.7% |
| Western Pacific and East Asia (Australia, NZ, China, Japan, S Korea) | 28.6% | 17% | 16% |
| SE Asia | 17.4% | 14.1% | 16.2% |
| Americas | 15.7% | 16.4% | 15.2 |
| Eastern Mediterranean | 2.9% | 13.4% | 16.4% |
| Africa | 0.8% | 10.6% | 16% |
Bone Health
The bones play a major part in the function of the body. In addition to being involved in structural support of the body, and in the protection of key organs, they also act as an area for the storage of minerals.
The bones themselves are largely composed of a protein called collagen and a crystal matrix of calcium-phosphate minerals; approximately 99% of the body’s calcium is stored in the bone tissue
In addition to the collagen and crystal matrix, bones also contain living cells. Many of these are involved in the bone remodeling cycle. This process involves the addition and removal of calcium by osteoblasts and osteoclasts. This process allows the body to remove calcium that is stored in the bones and release it into the blood stream when it is required for important processes such as nerve signaling.
When we are young, there is a net gain in bone mass as the skeleton grows. The addition of bone tissue continues after skeletal growth is complete, and most people gain peak bone mass in their early twenties.
Unfortunately, as we age, the bone remodeling cycle becomes less efficient and we begin to lose bone mass. Depending on one’s genetic makeup and lifestyle factors, the mass of the bones may remain constant, or steadily decline from the mid-twenties until mid-life. At this stage, an age-related loss of bone occurs in both men and women.
Once a woman reaches menopause, and for the following four to eight years, there is a marked acceleration in the rate of bone loss; this is typically between 1–2% per year. The rate of bone loss then slows down, so that typically men and women lose bone mass at similar rates once they have reached the age of 65.
Bone Density: Osteopenia and Osteoporosis Classification
Bone strength is related to its quality and density, and there is a strong correlation between bone mineral density and the risk of fracture.
- There is a marked increase in this risk of fracture with every standard deviation to the mean.
When people should have their bone mineral density tested varies from country to country, but the NOF[http://www.nof.org/] suggests the following people be tested:
- Women from the age of 65; Men from the age of 70.
- Menopausal and postmenopausal women, and men over the age of 50, who have osteoporosis risk factors, or have had a fracture.
- Women who are receiving medication for, or have a condition associated with bone loss.
The commonest used method for testing bone density is that of dual energy X-ray absorptiometry (DEXA; DXA). The DEXA scan procedure takes around 15 minutes, is painless, and uses a very low dosage of radiation.
Results are given as a T-score. This is based upon a standard deviation to the norm.
Historically, the WHO defined operatively osteoporosis as a variation of bone mineral density at the hip of 2.5 or more standard deviations than that of the mean value of a young Caucasian healthy women. Nowadays, measures are also taken at the lumbar spine and in men; and the reference is the mean value of young adults.
There are three main bone strength categories based on T-scores:
- Normal: A BMD T-score higher than –1
- Osteopenia: A BMD T-score of between –2.5 and –1
- Osteoporosis: A BMD T-score of below –2.5
In addition to the T-score, you will usually receive Z-score and FRAX score results following a DEXA test. The Z-score compares bone density with people of like-age, and is not relative to older people. The FRAX tool is used to give an estimate of the likelihood of a person breaking a bone in the following ten years.
Types of Osteoporosis
There are four major types of osteoporosis:
- Primary osteoporosis: this is the commonest form of osteoporosis and is a consequence of natural bone loss.
- Secondary osteoporosis: this type is related to having a medical condition, or through taking medicines known to break down bone tissue.
- Osteogenesis imperfecta (Brittle bone disease): this is a genetic disorder present at birth.
- Idiopathic juvenile osteoporosis[http://link.springer.com/article/10.1007%2Fs00223-001-0045-y?LI=true]: This condition is prevalent prior to puberty, and is of unknown etiology.
Types of involutional osteoporosis
There are two major types of involutional osteoporosis:
- Postmenopausal osteoporosis [type 1] – Affects only women. At the time of the menopause women experience a rapid increase in bone loss. Mainly affects trabecular bone.
- Senile osteoporosis [type 2] – Affects men and women. Attributed to ageing processes, such as the osteoblasts becoming dysfunctional. Affects both cortical and trabecular bone.
Signs and Symptoms of Osteoporosis
Unfortunately, the signs and symptoms of osteoporosis are not obvious, and the condition is usually diagnosed following a bone breakage. Here are some of the major indicators of the condition.
- Fragility/low impact fractures.
- Loss of height and/or stooping.
- Pain in the joints and/or bones.
- Dental X-ray.
See this page for more information on the symptoms of osteoporosis.
Fragility Fractures
A fragility fracture is a breakage that occurs as a result of a fall from a standing height or less. It is both a consequence of, and a known risk factor for, osteoporosis. Approximately 2.5 million fragility fractures occur in Europe per year, and 1.7 million in the USA. Over 80% of the fragility fractures that occur in people over the age of 50 are linked to osteoporosis.
Once a fragility fracture has occurred the risk of a second occurring increases dramatically. Osteoporosis Canada estimates that 14% of people with a wrist fracture will suffer a repeat within three years; ~33% with a hip fracture will repeat the injury within one year; and there is ~20% chance of a second spinal injury occurring within a year of the initial vertebral fracture.
Major Types of Osteoporosis Fractures
The most common types of osteoporosis fracture affect the wrists, spine and the hips.
Hip fractures
Fractures of the hip are especially of concern as this kind of injury can have serious consequences. It is estimated by the WHO that there is a ~20% lifetime risk of hip fracture in women over the age of fifty that live in developed countries.
Osteoporosis is responsible for around 70–90% of all hip fractures; and they are at their most prevalent in elderly people in their seventies and eighties. The survival rate from such a major injury is strongly correlated to the overall fitness of the person before the hip fracture occurred. Unfortunately, ~28% of women, and ~37% of men are likely to die within the 12 month period following an hip fracture (these figures are for Canada, and will vary from country to country, based on many things, especially the ability of a good health care system).
Wrist fractures
One of the first signs that someone has osteoporosis is often a result of a wrist fracture. This is because a person will instinctively reach out with their arms if they stumble and fall. As wrist strength will be lower in a person with osteoporosis, the bones will not be able to cope with the impact of the fall and results in a fragility fracture.
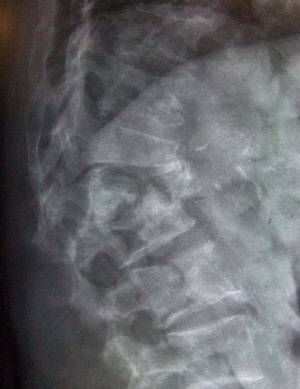
Spinal bone fractures
Spinal bone fractures (vertebral compression fractures) are the commonest type of osteoporosis fracture. These fractures usually occur in the lumbar (lower back) or thoracic (upper spine) regions.
When bone loses its strength the vertebra become narrower and shrink. This can lead to a loss of height or/and kyphosis.
As people with the skeletal disorder osteoporosis have weaker vertebra they are susceptible to spinal bone fractures when too much pressure is put on the skeleton. These often occur after an awkward movement, or when coughing or sneezing.
Spinal bone fractures often result in back pain; this is especially prevalent in the area close to the vertebral compression fracture itself.
Reducing the Risk of Fracture
Just because you have been diagnosed with osteoporoses does not mean that your bones will break. However, as you bone strength will be less than ideal you will be at an increased risk of fracture. One of the commonest ways that people with osteoporosis break bones is through falling. Wrist fractures often occur when a person reaches out to support themselves when they stumble.
Therefore, one of the best ways of avoiding a fracture is to improve one’s balance, and to be especially careful in situations where you are likely to slip, such as when getting out of a bath, or walking in icy conditions. In an ideal world, you will have someone with you to offer support when faced with slippery conditions (or perhaps carefully walk on grass verges), and have some sort of support rail fitted into the bathroom. Other recommendations to reduce the risk of a fall include using a cane/walking stick or walker; wearing shoes that have a good rubber grip; ensuring that any rug in the house has a rubber backing so that it does not slip; using a rubber bat/shower mat; and keeping the room free of clutter that you may trip over.
By improving your balance, you will be less susceptible to falling. Perhaps one of the best forms of exercises for elderly (and the young) is Tai chi (and other martial arts, for the younger ones who are looking for a preventative exercise). This exercise has been proven to improve balance, and led to a reduced incidence of fractures due to increased sway perimeters in research carried out in China.
Osteoporosis Risk Factors
There are two major classifications of osteoporosis risk factors. The first group includes factors that are outside of your control (non-modifiable) such as age, sex, body frame, menopause, family history. The second group includes things that you can control by making lifestyle choices (potentially modifiable), and includes factors such as diet, weight, exercise, smoking and alcohol consumption. A further risk group is related to medications, many of which are known to have side effects related to bone strength.
Even though you may be at risk from osteoporosis as a consequence of factors in the first group, by making lifestyle changes, such as consuming relevant nutrients, and partaking in weight bearing exercises you can dramatically improve your bone health in comparison to people in the same risk groups who do not make a conscious effort to deal with osteoporosis.

Go to this page for further information on osteoporosis risk factors.
Osteoporosis Treatments and Preventative Care
Depending on your individual condition, osteoporosis may be treated by medications and/or changes in life style such as an osteoporosis specific diet that is rich in minerals such as calcium, magnesium, manganese, zinc, and the vitamins D and K; and weight bearing exercises that are focused on strengthening bone. As medications should be avoided in general, ideally people would deal with osteoporosis by lifestyle choices from an early age.
Unfortunately, many people may need to take osteoporosis drugs to treat the condition. Although, there are some serious side effects associated with some of these medicines – there is a strong link between jaw necrosis, bisphosphonate use, and dental surgery – most osteoporosis drug side effects are minor and can be avoided through correct usage and regular consultation with your doctor/nurse.
The main drugs that are used for the treatment of osteoporosis are the bisphosphonates[JUMPLINK] (Aclasta; Actonel; Aredia; Bonefos; Boniva; Didronel; Loron; Fosamax; Nerixia; Skelid; and Zometa). Other osteoporosis medications in use include Calcitonin; Denosumab[JUMPLINK]; Estrogen replacement therapy; Parathyroid hormone; Selective estrogen receptor modulators; Strontium Ranelate[JUMPLINK]; and Tibolone.
Visit this page for more information on osteoporosis medications.
Summary
Osteoporosis is a condition characterized by a loss of bone strength. It affects both men and women, but women are at more risk of the condition. This is largely due to an increase in the rate of bone loss that occurs at, and after the menopause. Between 33%–50% of women, and 20% of men over the age of fifty are likely to fracture a bone due to having osteoporosis. The most common fractures that occur are of the spine, wrists, and hip. Osteoporosis is usually treated by medications and/or lifestyle changes; and often a combination of the two.